PhotoActivated PRP (PAPRP) – Enhancing the Effects of PRP

By exposing the PRP serum to light at specific frequencies, doctors create PhotoActvated PRP (PAPRP) that has enhanced therapeutic effects. Light stimulates the growth of additional compounds in the plasma that add to its healing mechanism. Tests conducted on patients with knee arthritis and injuries showed that PAPRP lowered pain and improved mobility.
Doctors have long been aware of the beneficial effects of light on tissues. Photoactivation or exposing soft tissues to light at specific wavelengths can speed up their healing processes. Keeping this principle in mind, PRP practitioners are exploring the use of PhotoActivated Platelet Rich Plasma (PAPRP) to help patients with joint pain and other musculoskeletal issues.
As the National Center for Biotechnology Information reports, by placing the PRP serum in a photoactivation device before injecting can possibly enhance its effects. The growth factors, mesenchymal cells, bioactive molecules, cytokines, and others healing components present in PhotoActivated PRP could work more efficiently resulting in the need for fewer follow-up sessions.

Healing Eroded or Damaged Cartilage Poses a Challenge
To date, there was no cure for arthritis or knee injuries because cartilage does not have the capability to repair itself. For this reason, you notice that knee injuries take a long while to get better and regain proper mobility. Here’s why:
- Like tendons, cartilage receives very little blood supply. And, without the boost of fresh oxygen and nutrients, this tissue is unable to heal.
- Whenever you have an injury and bleed, the blood forms a clot on the site. This clot contains the matrix that the damaged tissue uses to repair and heal. Since cartilage does not experience adequate bleeding when injured, it does not receive the growth factors, cytokines, and cell repair compounds produced in the body. With only the basic cells that create cartilage or chondrocytes to help, the tissue takes longer to heal.
PRP Treatments for Cartilage Repair Presented a Potential Cure for Arthritis
The discovery of PRP treatments for cartilage repair proved to be a boon for patients with joint pain resulting from eroded or damaged cartilage and buffering agents. That’s because the mesenchymal stem cells (MSC) contained in the PRP serum have the property of converting into chondrocytes. MSCs are created in the bone marrow and remain inactive until they reach the tissue site. By placing the MSCs with activating agents into the treatment site, doctors can stimulate the worn or damaged tissues to regenerate and repair.
In addition to chondrocytes and mesenchymal stem cells, PRP contains various other elements that can lower pain levels and reduce inflammation. These elements can also boost the production of lubricating or synovial fluids that cushion the joints and allow smooth movement.

PhotoActivated PRP Goes a Step Further
Combining the therapeutic effects of PRP injections for joint pain with photoactivation could enhance its regenerating powers. This mechanism occurs because the low-intensity light at specific frequencies used in PhotoActivated PRP can stimulate the release of more helpful components. These compounds include:
- Bioactive molecules that act on tissue helping it repair
- Beta-endorphins that provide relief from the pain
- Anti-inflammatory agents that help bring down the swelling (swelling interferes with the healing process of the cartilage)
Here’s How Doctors Prepare and Inject PhotoActivated PRP
- Lab technicians harvest 24 ml of blood from the forearm of the patient.
- After separating the blood into three portions of 8.5 ml each, the portions are placed in 3 BD Vacutainers. These test tubes contain ACD, a compound that prevents clotting.
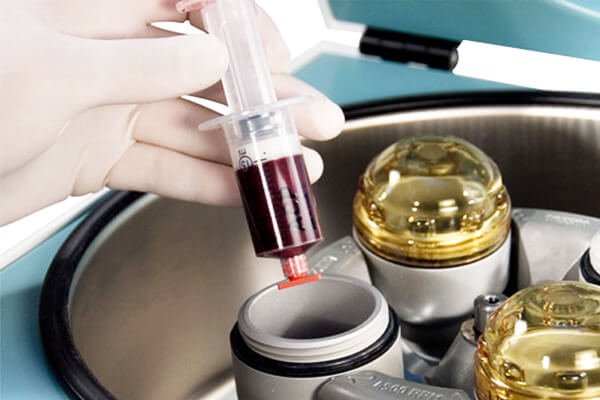
- Doctors spin the test tubes at 1000 RPM for 10 minutes. In response to the motion, the blood separates into 3 layers with the red blood cells settling at the bottom. The upper layers comprise of platelet poor plasma (PPP) and the buffy coat.
- Medical practitioners extract the buffy layer along with some of the PPP and 2 mm of red blood cells. They place the test tube containing this mixture into the photoactivation device for 10 minutes.
- Maintaining strict hygienic conditions, doctors place 4 mm of PhotoActivated PRP laterally into the knee of the patient. For precision with the placement, they use an ultrasonic imaging device. No painkillers were injected along with the PRP injection.
- The complete PAPRP treatment has three sessions given at intervals of one week.
Studies Have Proved that PhotoActivated PRP Works
Doctors conducted tests on patients that had osteoarthritis and painful knee injuries resulting from a basketball incident. They tested patients before and at 15 weeks after the completion of the PhotoActivated PRP course. They used tests such as:
- Numerical Pain Rating Scale (NPRS)
- Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC)
- 3-T MRI system scans
The results showed marked improvements in knee function and mobility with an 80% relief in pain. The patient that had opted for PRP treatment to help with the knee injury experienced a 100% relief from pain and discomfort during movement.
Doctors agree that more detailed testing is needed before they can conclusively declare that PhotoActivated PRP is effective. However, the preliminary results show that PAPRP could be the next step in PRP therapy.
If you’re interested in learning more about PhotoActivated PRP, feel free to contact us for more information. You can also call this number: (888)-981-9516. Our consultants can help you with all the details you need.
Have you tried PRP therapy before for any medical or cosmetic issues? Would you like to talk about how the treatment progressed and the outcomes? We’d love to hear about it. Please use the comment box below.
References:
Platelet-rich plasma therapy for a traumatic knee chondral lesion